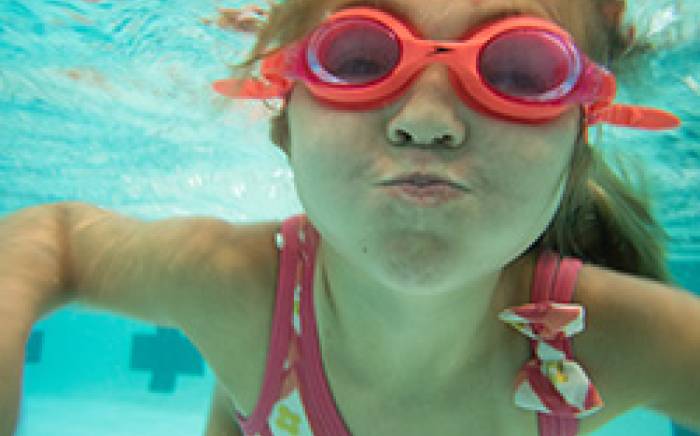What is the corpus callosum and how is it related to seizures?
The corpus callosum is a major structure permitting exchange of information between the two hemispheres, or halves, of the brain. In some children, seizures may spread from one hemisphere to the other through the corpus callosum. This may result in generalized seizures, including ‘drop attacks’ or atonic seizures.
What is a corpus callosotomy?
When patients with generalized seizures, and drop attacks in particular, fail multiple seizure medications, a corpus callosotomy may be considered. In this operation:
- The front 2/3rds, or in some cases, the entire corpus callosum is divided.
- The neurosurgeon can approach and divide the corpus callosum by operating between the two brain hemispheres, thus minimizing any potential injury to the brain.
- Alternative, minimally invasive approaches use Gamma Knife or laser thermal ablation (Laser interstitial thermal therapy: LITT) to ablate a section of the corpus callosum without open surgery.
Corpus callosotomy outcomes
While a corpus callosotomy does not ‘cure’ the seizures, 3/4s of properly selected patients enjoy an improvement in seizure frequency and severity. While drop attacks respond most favorably to this operation, other seizure types may also be improved. Major complications from this surgery are rare.
Corpus callosotomy procedure: what to expect
- The operation takes place under general anesthesia, and takes about four hours.
Usually a linear incision is used, over the top of the head. - A small window of bone is removed to perform the surgery, and then replaced after the corpus callosum has been divided.
- Absorbable sutures are placed in the skin, and the child is awakened in the recovery room.
- After overnight observation in the Intensive Care Unit, the child is transferred to our neurosurgery/neurology ward for an additional few days of recovery.
- Follow-up visits are scheduled 2-3 weeks after surgery, and again at 6, 12 and 24 months after surgery.
- The St. Louis Children's Hospital comprehensive epilepsy team has evaluated hundreds of children for this procedure, and has performed nearly 100 callosotomies as of 2017 without major complications.
Publications from our epilepsy team related to corpus callosotomy:
1. Palliative epilepsy surgery in Dravet syndrome-case series and review of the literature.
Dlouhy BJ, Miller B, Jeong A, Bertrand ME, Limbrick DD Jr, Smyth MD.
Childs Nerv Syst. 2016 Sep;32(9):1703-8. doi: 10.1007/s00381-016-3201-4. Epub 2016 Jul 27.
2. Outcomes after anterior or complete corpus callosotomy in children.
Kasasbeh AS, Smyth MD, Steger-May K, Jalilian L, Bertrand M, Limbrick DD.
Neurosurgery. 2014 Jan;74(1):17-28; discussion 28. doi: 10.1227/NEU.0000000000000197.
3. Palliative epilepsy surgery in Aicardi syndrome: a case series and review of literature.
Kasasbeh AS, Gurnett CA, Smyth MD.
Childs Nerv Syst. 2014 Mar;30(3):497-503. doi: 10.1007/s00381-013-2259-5. Epub 2013 Aug 16.
4. Resting-state activity in development and maintenance of normal brain function.
Pizoli CE, Shah MN, Snyder AZ, Shimony JS, Limbrick DD, Raichle ME, Schlaggar BL, Smyth MD.
Proc Natl Acad Sci U S A. 2011 Jul 12;108(28):11638-43. doi: 10.1073/pnas.1109144108. Epub 2011 Jun 27.
5. Complete versus anterior two-thirds corpus callosotomy in children: analysis of outcome.
Jalilian L, Limbrick DD, Steger-May K, Johnston J, Powers AK, Smyth MD.
J Neurosurg Pediatr. 2010 Sep;6(3):257-66. doi: 10.3171/2010.5.PEDS1029.
6. Radiosurgical posterior corpus callosotomy in a child with Lennox-Gastaut syndrome. Case report.
Smyth MD, Klein EE, Dodson WE, Mansur DB.
J Neurosurg. 2007 Apr;106(4 Suppl):312-5.