Medical treatment of brachial plexus palsy includes diagnosis, ongoing assessment, and appropriate therapy.
Initial Management
Medical treatment of brachial plexus palsy begins with the following steps:
- diagnosis by neurologic examination
- identification of associated injuries
- education of the family about the disease and therapy
- daily range of motion exercises
- monthly assessment of motor strength
- for infants with persistent weakness, referral to Brachial Plexus Center before 2 months of age
Assessment
The infant's muscle strength and arm and hand movements are measured every month during the first 6 months. We use three grading systems to document muscle strength and functions of the upper extremities.
Motor Strength Assessment Scale
The Modified British Council Scale for muscle strength, illustrated below, is used for semiquantitative assessment of an infant's muscle strength.
1 - No or trace muscle contraction
2 - Muscle contraction without gravity
3 - Muscle contraction against gravity
4 - Muscle contraction against resistance
NG - Not graded due to difficulties
This muscle strength grading system is applied to each muscle group of the affected upper extremity, as shown below:
| Muscle | Strength |
| Deltoid | |
| Shoulder external rotators | |
| Shoulder internal rotators | |
| Biceps | |
| Triceps | |
| Wrist flexors | |
| Wrist extensors | |
| Finger flexors | |
| Finger extensors |
Joint Movement Grading
This grading system allows for quantitative documentation of the joint movement.
| Observation | Central Grade | Numerical Score |
| No joint movement | 0 | 0 |
| Flicker of movement | 0+ | 0.3 |
| Less than half range | 1- | 0.6 |
| Half range of movement | 1 | 1.0 |
| More than half range | 1+ | 1.3 |
| Good but not full range | 2- | 1.6 |
| Full range of movement | 2+ | 2.0 |
(Note: The best movement observed during evaluation is graded.)
This joint movement grading system is then applied to specific movements of each joint of the affected upper extremity, and a total numerical score is found.
| Joint Movement | Central Grade | Numerical Score |
| Shoulder adduction | ||
| Shoulder abduction | ||
| Elbow flexion | ||
| Elbow extension | ||
| Wrist flexion | ||
| Wrist extension | ||
| Finger flexion | ||
| Finger extension | ||
| Total Numerical Score | ||
By recording these objective data for muscle strength and joint movement, a patient's progress can be followed through a series of examinations.
Click for larger image
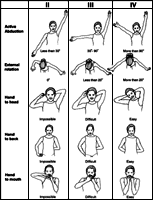
Mallet Scale
Another grading system to document functional changes of the shoulder and arm is the Mallet Scale, which is very useful in children older than two years. (Because it requires the cooperation of the patient, it is not suitable for younger children.) Click on the image to see a larger version.
Physical Therapy
In all infants with brachial plexus palsy, early therapeutic intervention is important. At the initial evaluation at the Brachial Plexus Palsy Center, physical and occupational therapists evaluate the infant as a team. Therapists instruct parents on home exercises and help set up regular local therapy, if necessary.
Exercises provided by the therapists are designed to help improve muscle strength, preserve flexibility and mobility of joints, and protect joint integrity. Splints may be recommended to help improve joint position, function and/or to stretch a tight muscle. The therapists concentrate on caregiver education and training because of the importance of understanding and doing the exercises several times a day at home.
For the child 3 years and older, recommendations for adaptive tools or instructions for alternative techniques for Activities of Daily Living (ADL’s) may be issued to help increase the child’s independence in various skills, such as self-feeding or dressing. The therapists may recommend community activities like swimming, dance, martial arts, musical instruments or adaptive bicycles. These activities can be motivating for children of various ages and levels of severity.
Physical therapy is the only treatment necessary under these conditions:
- The infant can bend the elbow against gravity and move the wrist and fingers by 3 months of age.
- Muscle strength continues to improve.








