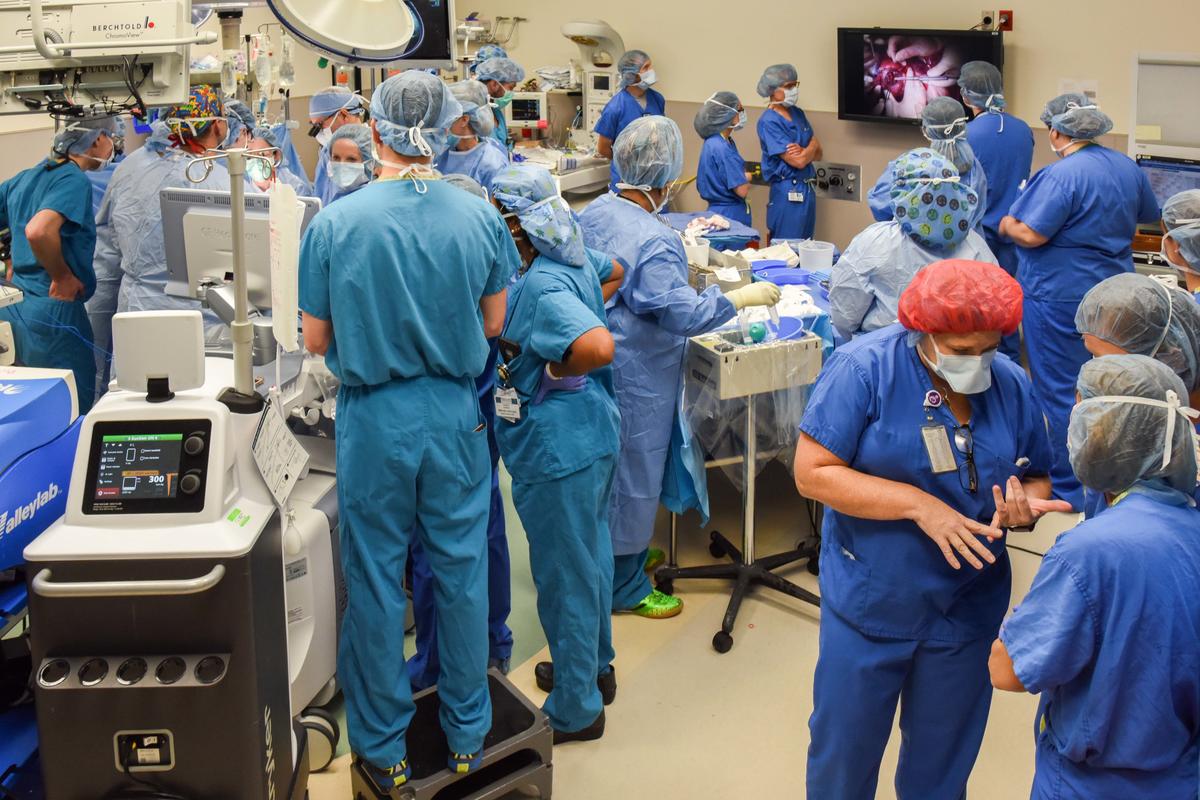
 In October, Washington University surgeons and physicians from St. Louis Children’s and Barnes-Jewish hospitals collaborated to perform a prenatal closure of a myelomeningocele in a 25-week-old fetus with spina bifida.
In October, Washington University surgeons and physicians from St. Louis Children’s and Barnes-Jewish hospitals collaborated to perform a prenatal closure of a myelomeningocele in a 25-week-old fetus with spina bifida.
In total, 35 medical professionals took part in the rare surgery that was the first of its kind at the Washington University medical campus.
“This was a significant event that has the potential for benefiting families throughout the Midwest,” says Michael Bebbington, MD, MHSc, director of the Fetal Care Center of Barnes-Jewish Hospital (BJH), St. Louis Children’s Hospital (SLCH) and Washington University School of Medicine. “Rather than traveling long distances, this advanced care now is available closer to home.”
Spina bifida occurs when the fetus’ spinal canal remains open along several vertebrae in the lower or middle back. This causes the membranes surrounding the spinal cord and some nerve fibers to protrude, forming a sac on the baby’s back. The condition may cause physical and neurological problems to the lower limbs, bowel and bladder, as well as hydrocephalus, for which a ventricular shunt is usually needed.
In years past, the standard of care for treating myelomeningocele was to perform neurosurgery, usually within 24 to 48 hours after birth. The procedure involved repositioning the exposed tissue back into the spinal column and covering it with muscles and skin.
In recent years, however, evidence has shown that in some cases fetal surgery for myelomeningocele may improve neurological outcomes. That was the finding of the Management of Myelomeningocele Study (MOMS), a randomized, multicenter clinical trial sponsored by the National Institutes of Health comparing the outcomes of prenatal surgery with postnatal surgery. The results of the trial were published in the New England Journal of Medicine in February 2011.
“The MOMS trial showed that for a select group of fetuses, in utero surgery can result in three major benefits,” says Dr. Bebbington, who participated in the clinical trial when he was at the Children’s Hospital of Philadelphia. “One is that the high-brain herniation occurring as a result of the lesion is reversed, meaning the cerebellum migrates back up into a more normal position. Second, the need for shunting because hydrocephalus is decreased by 50 percent compared to postnatal surgery. Finally, neurologic function may improve by up to two levels, which for some children means the difference between walking and not walking.”
According to Washington University neonatologist Barbara Warner, MD, co-director of the Fetal Care Center, a variety of problems can arise when children need shunting. Among these is shunt malfunction that requires revision surgery, a constant source of worry for parents.
“Eliminating the need for shunting is a significant improvement for patients with spina bifida and their parents and greatly enhances these children’s lives,” she says.
CAREFUL, HIGHLY SELECTIVE EVALUATION
The MOMS trial established particular inclusion/exclusion criteria that determine pregnant mothers and their fetuses’ eligibility for prenatal repair of myelomeningoceles. Among these are:
For fetuses (inclusions)
- Open neural tube defect between T1 and S1
- Evidence of a chiari malformation, the condition in which brain tissue extends into the spinal canal
- Singleton pregnancy between 19 and 25 weeks
- Normal karyotype
For mothers (exclusions)
- Factors that may increase risk for preterm labor and delivery; e.g., short cervix, uterine abnormalities, placenta previa, prior spontaneous preterm deliveries
- Major medical conditions such as diabetes, or infectious diseases that may be transmitted to the fetus during surgery
- Body mass index of more than 35
If the various initial criteria are met, families undergo an extensive evaluation, including specialized ultrasound study and a fetal MRI. The families then meet with Dr. Bebbington to review the results of the study, what that means for the developing fetus, and all the options for ongoing care. If they are good candidates for open fetal surgery, the next step is meeting with the pediatric neurosurgeon, pediatric surgeon, pediatric anesthesiologist and a social worker. Approximately one out of every five families evaluated is identified as good candidates for the surgery.
“We conduct psycho-social evaluations to ensure the mothers can cope with the stress and rigors of the surgery, and that they have support people available once they are discharged from the hospital,” says Dr. Bebbington. “Because of the nature of the surgery, the remainder of the mothers’ pregnancy care changes. The moms are on bed rest, and that means having someone with them at all times to help with their needs and, most importantly, that can get them to the hospital if need be.”
He adds, “The mothers can sometimes go back to their homes, but only if they live in close proximity to a large-enough medical center that has a specialist available to continue caring for them. Otherwise, they need to remain in St. Louis. We encourage families who have undergone open fetal surgery for myelomeningocele to return to St. Louis for delivery.”
Dr. Warner says those involved in the in-depth screening process act as stewards of careful evaluation of benefit. “As with all surgeries, in utero myelomeningocele spina bifida surgery carries certain risks to the mother and the fetus, and we are careful to make sure the parents understand these before they make a decision,” she says. “Parents can be easily swayed to want to do ‘everything’ for their baby, especially when new, life-changing procedures become available. In the vast majority of cases, myelomeningocele spina bifida is not a lethal congenital defect, but it can result in serious impairment and sequelae. All factors are weighed carefully before moving forward.”
THE SURGERY
Dr. Bebbington describes the October in utero surgery as a kind of “ballet,” with those present knowing their role and maneuvering through the operating room. In addition to the surgeons, those present during the three-hour surgery included a pediatric cardiologist, adult and pediatric anesthesiologists, a neonatologist, clinical pharmacist and a skilled team of operating room support staff.
The first step in the surgery was Dr. Bebbington and Washington University pediatric surgeons Jesse Vrecenak, MD, and Brad Warner, MD, opening the maternal abdomen and positioning the fetus inside the uterus so that the small section of the spine where the lesion was located was visible. At that point, Washington University pediatric neurosurgeons Jennifer Strahle, MD, and David Limbrick, MD, repaired the open neural tube defect, closing it with fetal skin; the amniotic fluid was reconstituted; and the maternal abdomen closed.
“Our multidisciplinary myelomeningocele clinic has a large number of resources we are able to deploy for our patients and their families,” says Dr. Strahle. “Although the success rates for this surgery are very impressive, ongoing success and sustained good outcomes for each mother and child requires ready access to care, a team that can respond to questions and changes as they arise, and guidance for families to help them anticipate milestones. Our team at Washington University is as well-prepared to do this as any institution I have seen.”
Following surgery, there is a four-day protocol of postoperative care because of the risks of these surgeries, in particular fetal well-being and the possibility of contractions and infection.
In this case, the parents moved to St. Louis to be close to the physicians and hospitals.
“The closest hospitals with similar programs such as ours are in Cincinnati, Denver and Houston,” says Dr. Bebbington. “Our proximity should encourage physicians to recommend to families that they be evaluated at the Fetal Care Center. Beyond offering in utero surgery, we can offer a comprehensive, specialized evaluation and can help to educate families about spina bifida, what to expect and what resources are available to them.”
Among those resources is the large myelomeningocele clinic at SLCH. “We are looking forward to carefully following babies who have undergone this in utero surgery and tracking their outcomes,” says Dr. Warner. “It’s an exciting prospect.”
For more information about this case or to speak with a member of the surgical team, call Children’s Direct at 800.678.HELP (4357).