At less than 4 months of age, Evan Wells was the first patient at St. Louis Children’s Hospital to receive a heart transplant from a donor with a different blood type. It’s called an ABO-incompatible heart transplant. Evan has type O blood and received a heart from a donor with type A blood. This rare procedure took place on August 31, and Evan is currently listed in critical but stable and improving condition in the pediatric intensive care unit (PICU).
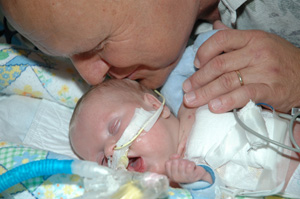 Evan was born with a heart defect called dilated cardiomyopathy. The left ventricle – the main pumping chamber of the heart – was enlarged and underdeveloped. It could not pump enough blood and oxygen to meet the needs of the baby’s tiny body.
Evan was born with a heart defect called dilated cardiomyopathy. The left ventricle – the main pumping chamber of the heart – was enlarged and underdeveloped. It could not pump enough blood and oxygen to meet the needs of the baby’s tiny body.
Many patients with cardiomyopathy respond to medications. However, in Evan’s case his heart failure developed inside his mother’s womb. It was detected by a fetal echocardiogram at St. Louis Children’s Hospital. His heart failure was so severe that it required an emergency C-section at 30 weeks. Since he was a pre-term infant and his heart was very small, he was listed as an ABO-incompatible heart transplant candidate so he would be eligible to receive organs from a donor with an incompatible blood type.
Due to the extreme scarcity of donor organs for infants, heart transplantation across ABO incompatibility has been considered for infants waiting for heart transplantation. Each year, 30 percent of the infants waiting for heart transplants die waiting. Around the world, there have been approximately 50 ABO incompatible transplants.
“The reason an infant can receive an incompatible heart transplant is that a newborn infant does not yet produce anti-A or anti-B antibody; blood group antibody production typically begins at about 6-8 months of age,” explains Charles Canter, MD medical director of the heart transplant program at St. Louis Children’s Hospital and professor of pediatrics at Washington University School of Medicine.
“Any organ transplant requires a strong clinical team working together, and in the case of this kind of innovative procedure, that teamwork in the post-operative period was essential and critical,” added Paul Checchia, MD section head, cardiac critical care medicine at St. Louis Children’s Hospital and assistant professor at Washington University School of Medicine.








