Riley Jones, 14, was born with three extra vertebrae that caused a sharp angular deformity of the spine and compressed her spinal cord. This congenital kyphosis was compounded by scoliosis and progressive growth during her pubertal growth spurt.
For many years, her condition didn’t stop her from being a star athlete in both soccer and basketball. “She could play basketball like nobody’s business,” says Riley’s father, Mark. “She scored 21 points in one game.”
But as Riley grew, her condition worsened. By age 12, pain and breathing issues forced her to quit soccer and basketball. “That’s when I realized how serious it was,” Riley says. “I started to hit my back on things and I couldn’t do as much with my friends anymore. I wore baggy clothes and wore my hair down to hide the point on my back.”
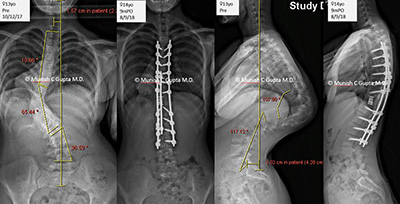
Riley also began experiencing pain and numbness in her back and legs, headaches, dizziness and back cramps. In addition, she was having difficulty breathing because her lungs were compressed. With severe congenital kyphosis, paralysis is a real possibility as the bent spine reaches 90 degrees or more.
An orthopedic surgeon near the Jones’s home in Indiana referred Riley to Munish Gupta, MD, a Washington University orthopedic spine surgeon specializing in spine deformity surgery at St. Louis Children’s Hospital. Dr. Gupta has been a spinal deformity surgeon for more than 20 years. He performs more than 150 spine surgeries each year.
Dr. Gupta and his colleagues, Mike Kelly, MD, and Scott Luhmann, MD, are some of the few surgeons in the Midwest who perform complex pediatric spinal deformity surgeries. They use 3D models in severe cases for surgery planning.
 “Every individual has a unique deformity," Dr. Gupta says. “X-rays don’t do the spinal deformities justice and even a CT scan is just not the same. For complex deformities, a 3D reconstruction allows me to better plan and prepare for surgery and helps me perform surgery more efficiently and safely. Before surgery, I can look at the model from all angles to see exactly where the anomalies are so we have fewer surprises. When you open the spine during surgery, it looks exactly as it did in the 3D model.”
“Every individual has a unique deformity," Dr. Gupta says. “X-rays don’t do the spinal deformities justice and even a CT scan is just not the same. For complex deformities, a 3D reconstruction allows me to better plan and prepare for surgery and helps me perform surgery more efficiently and safely. Before surgery, I can look at the model from all angles to see exactly where the anomalies are so we have fewer surprises. When you open the spine during surgery, it looks exactly as it did in the 3D model.”
He says 3D modeling allowed him to plan Riley’s complex surgery so he knew how to best correct the deformity, how much bone to remove, and to recognize the landmarks during surgery. “3D modeling has made pre-op planning and assessment of the deformity much better so we’re more comfortable going into the surgery. We know what we will find and can plan which pedicles we can put a screw into and which ones to avoid. When you’re relieving pressure on the spinal cord by removing bones or disc material, the risk of neurological injury is high so anything that makes surgery safer is a good thing.”
As 3D technology transforms health care and becomes more commonly used, St. Louis Children’s Hospital now has “in-house” 3D printing capabilities.
Located at the BJC Institute of Health on the Washington University Medical Campus, the Medical 3D Printing Center provides medical and surgical modeling using CT images or MRIs. Experienced bioengineers work with surgeons and other health care providers to develop custom, precision models of patient anatomy that accurately show the details and specific anomalies. These models allow physicians to tailor treatment plans to each patient.
“As the engineers have perfected the technology, the advanced 3D reconstruction now even shows where the rods, plates and bones are with different colors,” Dr. Gupta says.
Not all spine surgeons in the country use 3D models but Dr. Gupta hopes more surgeons will as the technology becomes less expensive. “3D models are an evolution in spinal surgery. Before, we just had X-rays. Next, we had CT images. And now we have 3D reconstruction on CT scans that we can make models from. The technology continues to evolve to include blood vessels on the models. This visualization gained through 3D models leads to a more successful outcome.”
Dr. Gupta performed Riley’s complex surgery in November 2017; it took nearly seven hours.
Now a freshman in high school, Riley is celebrating one year since her surgery. “As I look at the future, I know I can do what I want, I can wear anything, and I feel confident,” she says. “I can say nothing is wrong with me now and look forward to making fun memories in high school. I’m relieved and feel like I have this weight off my shoulders. I know I will never have pain like I did before surgery.”
Her parents are also relieved. “We knew Dr. Gupta was one of the top spine surgeons and we felt so comfortable with Dr. Gupta from the minute we met him,” Christy says. “The difference in Riley is like night and day since surgery. We’re so grateful.”
Mark agrees. “Before her surgery, we were worried she would have to spend her life in a wheelchair. We’re so happy to see her walking without pain now and breathing normally. She also came out of surgery 4 inches taller since her spine was straightened.”
Dr. Gupta says his goal is to educate more doctors about the value of 3D models and give hope to more patients. “It’s gratifying to see Riley have more self-confidence and feel better since we fixed the deformity. This surgery changed her life.”








