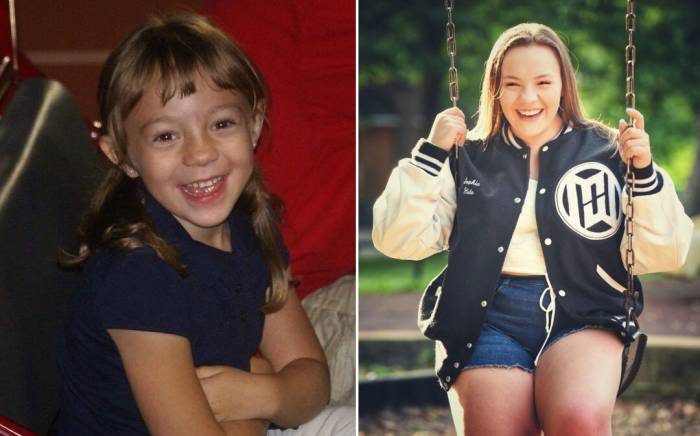SLCH Neurorehabilitation Program makes all the difference in epilepsy patient’s recovery
 When Cameron Schulze was 11 years old, he was an active kid who was living with epilepsy, but one February day turned Cameron and his family’s lives upside down for several months.
When Cameron Schulze was 11 years old, he was an active kid who was living with epilepsy, but one February day turned Cameron and his family’s lives upside down for several months.
Now 13 and in the seventh grade, Cameron has been a patient at St. Louis Children’s Hospital (SLCH) since he was just 3 weeks old.
“He’s had epilepsy since his first day of life,” says his mom, Becky, who along with her husband, David, and Cameron’s older brothers, Christopher and Nicholas, have been by their son and brother’s side as he dealt with constant seizures throughout his young life.
As a lifelong patient of Mary Bertrand, MD, a Washington University pediatric neurologist at SLCH, Cameron has undergone a series of treatments to address his seizures, which would vary at times from once a month to as many as 35 times a day. “Dr. Bertrand has never given up on Cameron. She always keeps trying things, and we love her,” Becky adds.
Cameron has undergone several surgeries at SLCH with Matthew Smyth, MD, a Washington University pediatric neurosurgeon, as well as at the Cleveland Clinic when Cameron was younger.
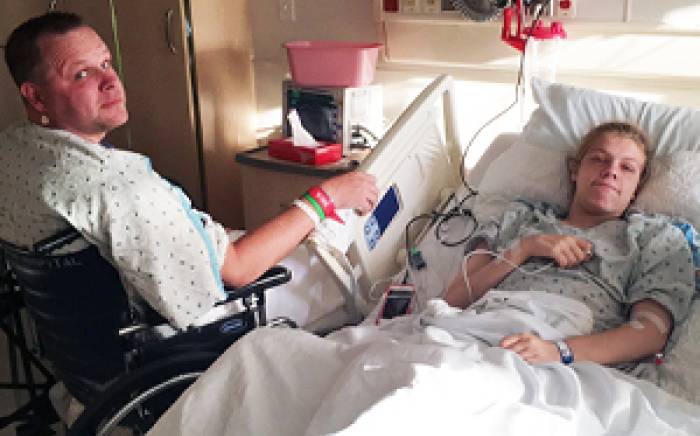
The Schulzes were always concerned about their son and how the seizures impacted him but never more so than on Feb. 18, 2015, when non-stop seizures led to an emergency room visit, hospital admission, and transfer to the pediatric intensive care unit (PICU) within a few days.
“Cameron was having seizures that were occurring continuously, and by Feb. 20, he was moved to the PICU, where he was put in an induced coma to try to stop them,” Becky recalls. “As a nurse, I knew how bad things really were, but the advantage was that I was able to ask a lot of questions. It was all very hard on our entire family, but I feel lucky we have such a comprehensive epilepsy program here at Children's Hospital.”
Six days later, Cameron underwent an emergency corpus callosotomy with Dr. Smyth. The surgical procedure is an operation that cuts the corpus callosum (the nerve fibers that connect the two hemispheres of the brain) in an effort to help lessen the severity of seizures.
“The corpus callosotomy was a really big surgery for Cameron,” Becky says. “We had a lot of faith in Dr. Smyth that he’d do a really good job, and he did.”
Cameron remained in the PICU for three weeks before being moved to the 12th floor and accepted to the hospital's neurorehabilitation program. It was there that he would have to relearn basic functional skills.
“Before all of this occurred, Cameron was a normal, functioning kid who was on a basketball team,” recalls Becky, who says by the time he was moved to neurorehab he had to relearn things like how to swallow, eat and sit up. “He was down to an infant level, but the neurorehab team never gave up on him. Their goal was to get him back to baseline.”
The neurorehabilitation program, under the leadership of Washington university pediatric neurologist Michael J. Noetzel, MD, is a comprehensive multidisciplinary team that includes specialized medical and nursing care, occupational, physical, speech therapy, child life and music therapists, and many other specialists dedicated to the care of children with neurological deficits. Most of the time, children receive therapy in the gym adjacent to the patient rooms. Children and families also enjoy access to many other resources, including the hospital’s schoolroom, playroom, teen lounge, Olson Family Garden, and Family Resource Center.
Therapeutic community outings are also planned by the care team for those children who are able to use newly learned skills in a natural environment. Outings may range from a visit to the Central West End neighborhood for ice cream to an outing at a local mall or the Saint Louis Zoo.
Cameron not only benefitted from his daily interactions with his therapists but also the many services provided by the hospital and the neurorehab team. One of the first therapists to interact with Cameron was speech language pathologist Erika Struckhoff, MA, CCC-SLP.
“I began working with Cameron while he was in the PICU. I was consulted the day after he was extubated to assess swallow safety and assist with communication, and continued to work with him after he was transferred to the neurology floor,” she says. “I saw him daily while he was an acute patient and 13 times a week once he was accepted to the inpatient neurorehabilitation program.
“Participating in speech therapy allowed Cameron’s diet to be advanced safely to the least restrictive diet for his skill level at the time. By the time he was discharged home, he was on a regular diet.”
Speech therapy was also necessary to help Cameron communicate effectively after his surgery and be able to express independently his wants and needs. Struckhoff explains that various speech therapy interventions were used to help Cameron, including swallow therapy, articulation therapy and cognitive therapy.
Cameron’s physical therapy sessions were led by Toni Goelz, PT, who first focused on helping him sit up using a chair with a tray to provide support. Since he was totally dependent like an infant, Goelz says they followed the same sequence an infant might by working on holding up his neck, sitting up and ultimately walking using a gait belt and then a walker.
“When he first started, his strength on his right side was at 20 percent, but by the time he went home in early April, his strength was at 60 percent, and he was walking and going up and down stairs,” Goelz says. “The next time I saw him after discharge from the hospital was a year-and-a-half later at our annual neurorehab reunion. If I had not seen his dad, I would not have recognized Cameron. He has done so well.
“There is a lot of satisfaction for all us to be able to work with children like Cameron,” she adds. “It’s so rewarding to see how they are doing.”
Although Cameron’s prognosis is unknown and he will require medications the rest of his life, his mom says he is doing very well.
“He hasn’t had a seizure since April 2016, and that is the longest he’s ever gone without one. He’s back to school, on a basketball team again and has no limitations,” Becky says. “Cameron is back to where he is 100 percent because of neurorehab and everyone at St. Louis Children’s Hospital.”
To speak with a member of the neurorehabilitation team at St. Louis Children's Hospital, call Children's Direct at 800.678.HELP (4357).