The following case study was used by Andrew J. White, MD, the James P. Keating, MD Professor of Pediatrics and division director of pediatric rheumatology, Washington University School of Medicine, and director of the St. Louis Children’s Pediatric Residency Program, as part of the “Patient of the Week” (POW) series. Many of the POW case studies cover uncommon illnesses, or common illnesses with unusual symptoms that can be overlooked. If you would like to be added to the POW email distribution, send an email to [email protected].
HPI: 7-year-old boy with autism, with a CC: abdominal and extremity pain. On 12/27/15 he began having trouble walking and would hold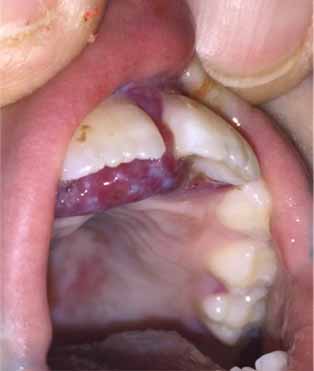 onto things like chairs or a railing. This progressed over two weeks to the point where he refused to walk at all. He complained of pain in his legs (all over), left wrist, ankle and toes, and he would occasionally point to his lower abdomen. Acetaminophen helps somewhat with the pain. There has been no trauma or injury. He has been receiving physical therapy without improvement. For the last two weeks has had increasingly loose stools and poor p.o. intake. He now is carried to the toilet, and when there, he appears flushed and has tremors and screams during attempts at defecation. He has also started picking at his gums, which is new for him; he normally picks at his earlobes and fingers, causing areas of
onto things like chairs or a railing. This progressed over two weeks to the point where he refused to walk at all. He complained of pain in his legs (all over), left wrist, ankle and toes, and he would occasionally point to his lower abdomen. Acetaminophen helps somewhat with the pain. There has been no trauma or injury. He has been receiving physical therapy without improvement. For the last two weeks has had increasingly loose stools and poor p.o. intake. He now is carried to the toilet, and when there, he appears flushed and has tremors and screams during attempts at defecation. He has also started picking at his gums, which is new for him; he normally picks at his earlobes and fingers, causing areas of
excoriation and bleeding. He has not had fevers, cough or rhinorrhea, no nausea or vomiting, no dysuria. He was seen by orthopedics three weeks before admission; X-rays taken were negative. When the refusal to walk continued, an MRI was performed; his lumbosacral spine and brain were normal. Physical therapy was initiated without improvement. A neurologist also evaluated him and prescribed baclofen and tizanidine, which have not improved his symptoms. He was seen by a second neurologist on the day of admission, who referred him here.
PMH: Autism, diagnosed at 2.5 years old. No CMA or Fragile X testing.
Social history: Limited diet. He eats only Chips Ahoy cookies, M&M’s, crackers with peanut butter and eclairs.
Developmental history: Able to say a few phrases. Prior to the events leading to this admission, had been running and walking independently, able to ride a scooter.
Physical Exam: Temperature 37.6, heart rate 130, respiratory rate 20, blood pressure 121/80, Sp02 98 percent.
General – Distressed and repeating phrases but lying in bed comfortably.
Skin – Warm and dry. Capillary refill less than 2 seconds. Rash on cheeks and bilateral shins. Excoriated patches on right ear and several fingers.
HEENT – Normocephalic, atraumatic. Conjunctivae clear without injection or scleral icterus.
Mouth – Gums with beefy red, hypertrophied excoriations, without drainage.
Neck – Supple without lymphadenopathy.
Lungs – Clear to auscultation bilaterally.
Cardiovascular – Regular rate and rhythm.
Abdomen – Soft, nontender, nondistended, normoactive bowel sounds.
Neurologic – Awake, alert, anxious.
Extraocular movements intact. Face symmetric. Normal sensation and strength on face. Normal strength of shoulder shrug. Moves all extremities against resistance. Keeps left upper extremity held against body with minimal movement. Increased tone in lower extremities. Achilles contractures. Keeps knees flexed. Resists extension. Full sensation to light touch in all four extremities. Reflexes 2+.
Course:
Vitamin D was 38, CK 131, CRP 39, ESR 68, CMP within normal limits, CBC with hemoglobin of 7.7mg/dL, microcytic.
Rheumatology was consulted and suspected vitamin C deficiency. Vitamin C level was drawn.
MRI of the lower extremities demonstrated abnormal signal enhancement in the lower extremity metaphyses and subperiosteal fluid in distal femurs; classic findings for scurvy. The white metaphyseal band visible on the plain film is also classic.
He was treated with IV vitamin C and had brisk and dramatic improvement in his pain. Resorption of the gum hypertrophy and hemorrhage was rapid. Pain resolved, and he had improved range of motion and use of his wrist. He had continued difficulty walking due to the flexion contractures of his knees.
Nutrition, speech and psychology were involved to help with his food aversion, and physical therapy to improve his range of motion.
Discharge diagnoses:
1. Scurvy (Vitamin C aka ascorbic acid deficiency) ICD-10 = E54.
2. Autism spectrum disorder.
3. Flexion contractures, knees, ankles, secondary to disuse.
4. Anemia, iron deficiency.
Discharge medications:
1. Ascorbic acid 150 mg p.o. two times daily.
2. Multivitamin with iron, one chewable tablet p.o. once daily.
3. Melatonin 6 mg p.o. once daily at bedtime.
4. MiraLAX 8.5 g p.o. once daily in the morning.
Comments: Scurvy is a rare disease in developed countries, but it continues to exist here in the United States. Lower extremity pain, limp and refusal to walk are the most common presenting complaints, and the diagnosis may be missed by most physicians not attuned to vitamin deficiency. Co-morbid conditions such as oral aversion, autism spectrum disorder, or any form of nutritional neglect, should be a big clue. Treatment includes not only vitamin C supplementation but also correction of underlying conditions in order to prevent recurrence. This particular patient will most likely have continued aversion to certain food products, and all options for providing the necessary nutrients should be entertained.