 The following case study was used by Andrew J. White, MD, the James P. Keating, MD, Professor of Pediatrics and division director of pediatric rheumatology, Washington University School of Medicine, and director of the St. Louis Children’s Pediatric Residency Program, as part of the “Patient of the Week” (POW) series. Many of the POW case studies cover uncommon illnesses, or common illnesses with unusual presentations. If you would like to be added to the POW email distribution, send an email to [email protected].
The following case study was used by Andrew J. White, MD, the James P. Keating, MD, Professor of Pediatrics and division director of pediatric rheumatology, Washington University School of Medicine, and director of the St. Louis Children’s Pediatric Residency Program, as part of the “Patient of the Week” (POW) series. Many of the POW case studies cover uncommon illnesses, or common illnesses with unusual presentations. If you would like to be added to the POW email distribution, send an email to [email protected].
Chief Complaint
Shortness of breath
History of Present Illness
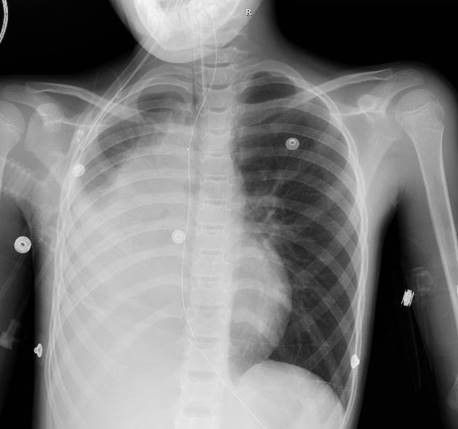
A 9-year-old with pectus excavatum presented to a local hospital with respiratory distress. She awoke 2 days prior to presentation saying that she couldn't breathe and had to throw up. Her sister has asthma, and albuterol at home, so she was given an albuterol treatment and her symptoms improved. She went to school and participated in regular activities. After school, she awoke from a nap with shortness of breath and a high-pitched loud breathing sound. She didn't improve with a second albuterol treatment, so parents brought her to the hospital where her oxygen saturations were in the mid-80s on room air. She received a third albuterol treatment and a chest X-ray was read as a RML pneumonia with tracheal deviation. She was given one dose of ceftriaxone and was transferred to an outside teaching hospital, where she was started on scheduled albuterol. There, pulmonology was consulted and recommended a CT scan, but she needed oxygen while lying flat to maintain acceptable O2 saturation. Flex bronchoscopy was performed, and she was transferred back to their PICU, intubated. The decision was then made to transfer her to St. Louis Children’s Hospital.
She has not had any recent fevers, weight loss, or night sweats. She has had a dry cough. No hemoptysis, chest pain, back pain. She did not recall any choking or aspiration events, but she did have corn for dinner a few nights ago.
Patient History
- Past Medical History: One prior abscess, pectus excavatum with restrictive lung disease
- Family History: Asthma, obstructive sleep apnea
- Social History: Lives at home with parents and 4 siblings. No pets or recent travel.
- Exam performed at St. Louis Children’s Hospital
- Vital Signs: T 37.6C | HR 110 | RR 33 | BP 119/92 | SpO2 93% on ventilatory support with an FiO2 of 100%
- General Appearance: Sedated and intubated
- Neck: No lymphadenopathy
- Pulmonary: Coarse, diminished breath sounds on the right. No audible wheeze or crackle. Pectus excavatum.
Select Labs:
- Respiratory viral panel negative
- CBC 15.2 > 14.5 < 349
- ABG 7.38/43/61
- LDH 482, uric acid 2.2
Differential Diagnosis:
- Pneumonia
- Foreign body aspiration, leading to obstruction
- Mediastinal mass, e.g., lymphoma
- Primary pulmonary tumor
- Granulomatous disease
Imaging:
A CT scan was obtained…and read as: "Abrupt cut off of the right mainstem bronchus just below the carina without tapering with an apparent enhancing endobronchial mass. Severe volume loss in the right hemithorax and consolidation of the entire right lung that is favored to represent a combination of severe atelectasis and postobstructive pneumonia. No definite mediastinal, hilar, supraclavicular, or axillary lymphadenopathy. Severe pectus excavatum deformity."
Course:
ENT performed a direct laryngoscopy and bronchoscopy. A soft tissue mass completely occluded the right mainstem bronchus, that appeared to be arising from the RUL bronchus. They began piecemail debulking of the mass. Once at the RUL takeoff, the mass was almost totally occluding the bronchus. An intraoperative consult to pediatric surgery was obtained and the team elected not to attempt further debulking due to risk of bleeding and difficulty accessing the entire mass.
Frozen section from the case was consistent with a granular cell tumor. Additional pathologic examination indicated a differential diagnosis of granular cell tumor versus alveolar soft part sarcoma (ASPS). Staining was non-confirmatory, given that granular cell tumors typically stain positive for S-100 protein and sarcomas are rarely endobronchial. Molecular studies were sent to determine the presence of the i(X;17) translocation, which is characteristic of ASPS, but was negative.
Diagnosis:
Granular Cell Tumor, S-100 negative, endobronchial, right upper lobe
Course:
- She was extubated on the day after her initial debulking procedure and rapidly weaned to room air.
- A PET CT did not identify any additional tumors.
- PFTs showed an FEV1 of 47%, FVC 49%, and FEV1/FVC 96%, consistent with her known restrictive pattern.
- One month later, she underwent bronchoscopy with right thoracotomy, and definitive resection of the RUL mass.
- Repeat PFTs showed an FEV1 of 89% predicted with an FEV1/FVC of 90%.
Comments:
Granular cell tumors are uncommon, usually benign (0.5-2.0% are malignant) tumors.
Treatment is surgical and is generally successful without recurrence. They appear to arise from Schwann cells, although in the past they were thought to arise from myoblasts. Clinically, they manifest on any skin or mucosal surface, and are often (40% in some reports) on the tongue (and up to 70% in the oral cavity). The tumor cells usually express S100 and CD68
The name is sometimes confused with granulosa cell tumors, which are malignant (usually) tumors that arise from granulosa cells in the ovaries or testes.
This case highlights the importance of a multidisciplinary approach. Input from the critical care and anesthesia teams were important for early airway management and ventilatory management strategies, as this patient essentially had single-lung physiology. Radiology, otolaryngology, pulmonology, pediatric surgery, and cardiothoracic surgery expertise were all necessary for optimal surgical approach and post-operative monitoring. Pathology and hematology/oncology were crucial for accurate diagnosis and future surveillance.
(Also on the differential was the most common primary lung malignancy in children, a bronchial carcinoid tumor, which often present with recurrent pneumonias due to obstruction by the carcinoid tumor. And while carcinoid syndrome can cause wheezing and cough in addition to the characteristic flushing and diarrhea due to systemic serotonin release, carcinoid syndrome is rarely encountered in lung neuroendocrine tumors and typically occurs in patients with disseminated disease or large primary tumors.)
References:
- Stieglitz, Franziska, et al. "Granular cell tumor of the trachea in a child." The Annals of thoracic surgery 79.2 (2005): e15-e16.
- Abdulhamid, Ibrahim, and Raja Rabah. "Granular cell tumor of the bronchus." Pediatric pulmonology 30.5 (2000): 425-428.
- Le, BH, Boyer, PJ, Lewis, JE, Kapadia, SB, Ganular cell tumor: immunohistochemical assessment of the inhibin-alpha, protein gene product 9.5, S100 protein, CD68 and Ki-67 proliferative index with clinical correlation. Ach Pathol Lab Med; 128(7):771, 2004.
- Solomon, LW, Velez, S-100 Negative Granular Cell Tumor of the Oral Cavity, Head Neck Pathol; 10(3):367, 2016. Potter, Samara L., et al. "Pediatric Bronchial Carcinoid Tumors: A Case Series and Review of the Literature." Journal of pediatric hematology/oncology (2018).
- Broaddus, Russell R., Cynthia E. Herzog, and M. John Hicks. "Neuroendocrine tumors (carcinoid and neuroendocrine carcinoma) presenting at extra-appendiceal sites in childhood and adolescence." Archives of pathology & laboratory medicine 127.9 (2003): 1200-1203.
- Spunt, Sheri L., et al. "Childhood carcinoid tumors: the St Jude Children's Research Hospital experience." Journal of pediatric surgery 35.9 (2000): 1282-1286.
- Gustafsson, Bjorn I., et al. "Bronchopulmonary neuroendocrine tumors." Cancer 113.1 (2008): 5-21.