The following case study was used by Andrew J. White, MD, the James P. Keating, MD Professor of Pediatrics and division director of pediatric rheumatology, Washington University School of Medicine, and director of the St. Louis Children’s Pediatric Residency Program, as part of the “Patient of the Week” (POW) series. Many of the POW case studies cover uncommon illnesses, or common illnesses with unusual presentations. If you would like to be added to the POW email distribution, send an email to [email protected].
CC: Rash
HPI: 3-month-old boy with two weeks of a worsening rash. It started around his mouth, and mom thought it was irritation from the “slobber” from his pacifier. It started to spread and a new “raspiness” to his cry prompted a visit to an urgent care center, where he was diagnosed with impetigo and started on an oral antibiotic and topical mupirocin. He had been afebrile, maintaining good PO, no URI symptoms, no respiratory distress, no vomiting/diarrhea.
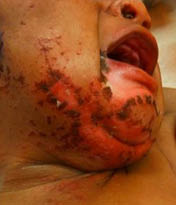 The rash did not improve, so he was brought to the ED.
The rash did not improve, so he was brought to the ED.
He has been breastfeeding well since birth, although he is small (25 percent).
ROS: No hair loss, no diarrhea or vomiting. FH: No similar rashes in siblings.
Exam: General – alert, active, healthy-appearing African-American male infant. T-37.2, RR 38, HR 110, normocephalic head shape. Anterior fontanelle was soft and flat. Hair distribution normal. Areas of skin breakdown and scaling in the scalp over the occipital region. The pupils were equal and round. Extraocular muscles intact. Nose and mouth were normal. He had no dentition. Palate was intact and normally shaped. Ears were normally formed. However, the skin of the face showed a rash around the mouth with a denuded area surrounded by crusty, dark-black scaling. He also had rash on his ears and around his eyes, as well as on his chin and upper neck. Chest shape was normal. Lungs were clear. He had a regular heart rate and rhythm with no murmur. His abdomen was rounded and soft with no organomegaly. GU was circumcised male with testes descended bilaterally. He had a rash in the diaper area. The limbs were normally formed. He had rash involving the elbows of both arms and a couple of patches of involvement on the skin of his fingers. The lower extremities were spared from rash. Neurological examination was unremarkable.
Diagnostic considerations:
1. Zinc deficiency a. congenital, aka Acrodermatitis enteropathica, aka Danbolt-Closs syndrome, aka Brandt’s syndrome b. acquired (malabsorption [CF, celiac], inadequate intake)
2. Biotin deficiency (also has a classic perioral rash)
3. SSSS (lack of a more disseminated rash makes staph toxin mediated disease less likely)
Investigations:
1. Alkaline phosphatase level (this zinc-dependent enzyme is low in zinc deficiency and returns quickly from the lab)
2. Zinc level
3. Biotin level
4. Sweat chloride
5. Sequencing of the SLC39A4 gene
Results:
1. Alk Phos was low (AlkPhos 60 Units/ml . . . normal range is 110 - 320 Units/ml)
2. Zinc was low (Zinc = 0.18 mcg/ml . . . normal range is 0.6 – 1.2 mcg/ml)
3. SLC39A4 is pending
Treatment:
1. Zinc sulfate (or gluconate, which is often better tolerated), 3 mg/kg per day
Comment:
Acrodermatitis enteropathica is the clinical syndrome of zinc deficiency (rash, diarrhea, alopecia and poor weight gain) caused by defects in the SLC39A4 gene (autosomal recessive), although the term is often applied to dietary zinc deficiency as well. The skin findings are typically present around the mouth, in the perianal area and in an acral distribution (hence the term) and can be confused with diaper rash or eczema. Dietary causes are typically due to malabsorption syndromes such as cystic fibrosis, and have even been reported in several cases of celiac disease. Treatment is supplementation with zinc, which makes sense for the acquired forms, but also works (for unclear reasons) for the congenital form. Recall that the SLC39A4 gene encodes a transmembrane protein that functions as a zinc transporter and allows the absorption of zinc from the GI tract. Clearly, however, oral zinc supplementation is able to overcome the defective transporter and correct the deficiency. Zinc is better absorbed from breast milk than from formula, affecting the age of presentation (bottle fed infants present earlier in life than breastfed infants). Zinc is present in meat and shellfish, but not in most plant products, leading some to estimate that nearly 2 billion people suffer from zinc deficiency worldwide.








