The following case study was used by Andrew J. White, MD, the James P. Keating, MD Professor of Pediatrics and division director of pediatric rheumatology, Washington University School of Medicine, and director of the St. Louis Children’s Pediatric Residency Program, as part of the “Patient of the Week” (POW) series. Many of the POW case studies cover uncommon illnesses, or common illnesses with unusual presentations. If you would like to be added to the POW email distribution, send an email to [email protected].
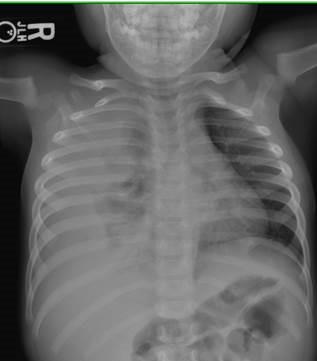 HPI: 19-month-old boy with asthma presents with fever and rapid breathing.
HPI: 19-month-old boy with asthma presents with fever and rapid breathing.
He felt warm the past six days (did not take temp) and for the past three days has had rapid breathing, wheezing and grunting. Mom gave nebulized albuterol, which helped initially but no longer helps. He also has clear rhinorrhea, NBNB emesis x1. Denies cough. Denies diarrhea. Decreased PO intake of food but good PO intake of liquid and good UOP. In ED he was febrile with RR 70s. He was given acetaminophen and once he defervesced, he improved.
CXR showed pneumonia. He was started on ampicillin, IV fluids and admitted to the floor.
PMH:
1. Behind on immunizations. Up to date as of 9 months.
2. Asthma. Home nebulizer.
Exam:
Vital signs 37.1, 131, 40, 103/83, 98%
Comfortable and in no distress. Skin warm and dry, no rash. Posterior pharynx clear, mucous membranes moist. No tonsillar hypertrophy. Neck supple, no lymphadenopathy. Crackles and diminished breath sounds on R, normal breath sounds on left side. No wheeze, no stridor. Soft, non-distended abdomen, non-tender, no hepatosplenomegaly, no masses, normoactive bowel sounds. Spine straight with no deformities visualized No clubbing, cyanosis or edema. CNs normal, moves all limbs.
CXR:
Admitting Assessment: “19 month old with six days fever and three days respiratory symptoms—wheeze, grunting, shortness of breath, no cough. Symptoms initially responsive to albuterol, but now with little response. Most likely diagnosis is community-acquired pneumonia. Differential also includes aspiration pneumonia and foreign body aspiration. Patient currently appears well when afebrile, worse appearing when temperature rises. No supplemental O2 currently.”
Plan:
1. Ampicilllin IV
2. Surgery consult for chest tube placement
A Diagnostic Clue: When the teaching attending was observing a medical student perform an H & P on this child, a clue was uncovered. Mom mentioned they had moved here seven months ago. “From where?” “A small town in rural Texas.” “Why?” “Dad is in and out of prison.”
Additional diagnostic consideration: Tuberculosis
Course: As the patient was about to head to the operating room shortly, the team moved quickly to notify infectious diseases and the operating room and the surgeons, who were able to successfully perform the procedure (chest tube) in negative pressure isolation and with appropriate protective gear (N95 masks), preventing what would have been exposure of many individuals to TB.
Results: PPD was positive at 18 x 20 mm. Antituberculous therapy was initiated, chest tube was removed after three days, and the patient improved and was discharged home after a week.
Treatment:
1. Isoniazid, Ethambutol, Rifampin, Pyrizinamide and B6 for two months, followed by two drug therapy for four months.
2. Notification of Department of Health.
Lessons:
1. Think TB
2. Retelling of the story, as is done in teaching hospitals, sometimes leads to new clues, and shouldn’t be viewed as onerous to family/patient/physician... instead, it can be useful.