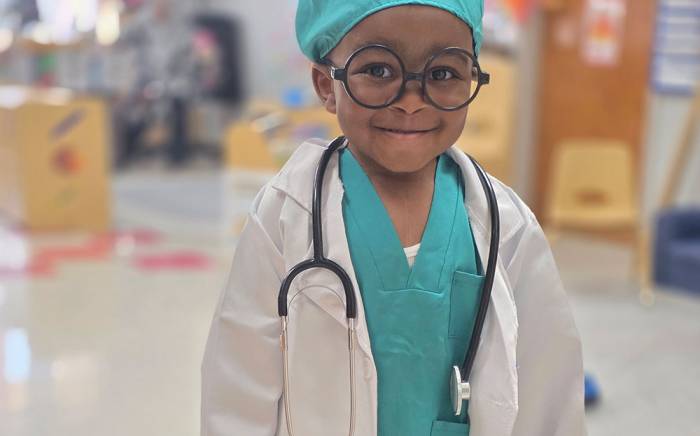
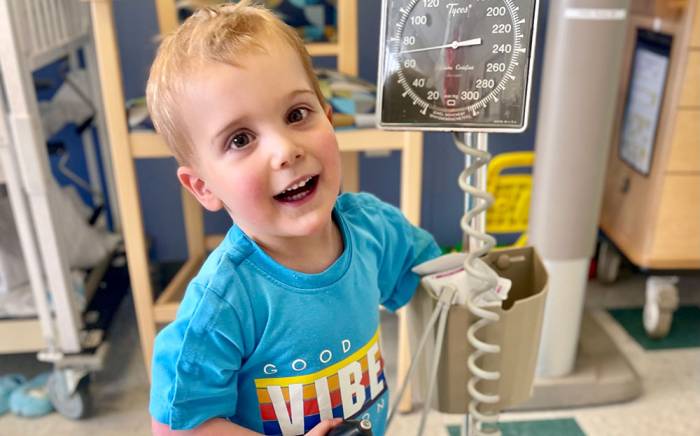
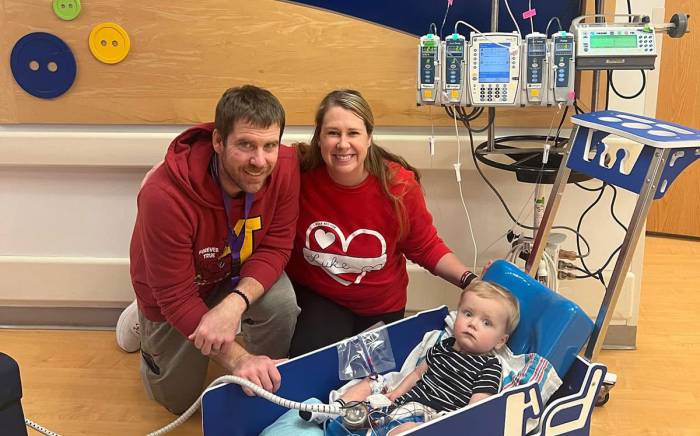
Samantha Etheridge is making sure her children have a normal childhood.
For Lynnleigh, 11, and Grayson, 6, normal means school, sports — and sleeping with an automated external defibrillator nearby to shock their hearts into beating regularly.
Samantha and her children have a rare, and potentially life-threatening disease called Brugada syndrome. Brugada syndrome is caused by a defect that can cause a disruption in the heart’s normal electrical activity, leading to arrhythmias.
A heart arrhythmia is when the heart’s electrical impulses beat either too fast or too slow, resulting in an irregular heartbeat. With Brugada syndrome, patients are at risk for fast, irregular rhythms originating in either the top or bottom chambers of the heart. This can cause the heart to stop pumping effectively and lead to a cardiac arrest.
Diseases like Brugada syndrome are called channelopathies. Channelopathies can occur as an isolated case in a single individual or can be found in multiple family members, like in the Etheridge family.
Brugada syndrome patients can experience symptoms including dizziness, fainting and seizure-like episodes. Unlike other channelopathies where symptoms often happen with exercise or during periods of high adrenaline, patients with Brugada syndrome most often have symptoms during rest or sleep that can occur without warning.
Samantha Etheridge had recurring fainting episodes while growing up but wasn’t diagnosed with Brugada syndrome until about five years ago — after she fainted getting up from the breakfast table one morning. She was successfully resuscitated, but that event prompted the work up that led to her diagnosis.
Because the condition can be inherited both Lynnleigh and Grayson were evaluated by pediatric cardiologists and geneticists, and were found to have the disease, too. Etheridge presumes the loss of a child several years previously was also a result of Brugada syndrome.
Being told you have a life-threatening heart condition is frightening. Being told your children have inherited it is even more so.
But there is an upside: Knowing that you have the diagnosis means you can take steps to prepare and minimize the risk. Understanding situations and conditions which may increase your risk of having an adverse cardiac event can help you make plans.
For example, pediatric patients with Brugada syndrome are at higher risk for adverse cardiac events when running a fever, and adults could be at higher risk if they are inadvertently exposed to certain medications that increase arrhythmias. Aggressive fever management in children with Brugada syndrome and avoiding medications on the Brugada drug list are part of the prevention and management strategy patients are taught.
Understanding situations that increase the family’s risk has allowed Samantha to feel good about the choices she is making for her family: for Lynnleigh and Grayson, that means participating in baseball, softball and volleyball. Lynnleigh, who’s “into horses,” has recently started riding lessons.
But since patients with Brugada syndrome are at a real risk for potentially deadly arrhythmias, a safety plan needs to be in place.
Etheridge had an internal cardioverter defibrillator (ICD) implanted in her chest. That is a device that detects and corrects irregular rhythm by delivering an electrical shock.
But that’s not an option for Lynnleigh and Grayson — yet.
Both children are seen in the St. Louis Children’s Hospital Inherited Arrhythmia Clinic by a multi-disciplinary team specializing in heart rhythm disturbances.
The clinic provides multidisciplinary care for the whole family with a team of electrophysiologists, geneticists, genetic counselors, and psychologists. The team works together to screen and identify affected family members and offer comprehensive care – addressing both the medical and psychological effects such a diagnosis can have on a family.
The children are currently being closely monitored with routine follow up, assessing their risk and potential need for an ICD. Both children have had implantable loop recorders (ILRs) inserted under their skin that allow the medical team at St. Louis Children’s Hospital to review recorded rhythms. If a life-threatening arrhythmia is identified, their care can be escalated, says Children’s electrophysiologist Aarti Dalal, DO.
But the decision to implant an ICD must be balanced with the patient’s size and clinical need for one, say their doctors. So, until Lynnleigh and Grayson have ICDs placed, the Etheridges rely on an automated external defibrillator (AED) to protect them.
The automated external defibrillator (AED) has the ability to do exactly what Samantha’s ICD can do: shock their child’s heart back into an organized rhythm.
The Etheridges received their AED from the Ollie Hinkle Heart Foundation, a St. Louis non-profit that partners with the Heart Center to provide services to children with congenital heart disease and their families.
“When we heard about Samantha and her family’s story, we automatically wanted to help. A big part of our mission is strengthening heart families through loving support, and we were honored to provide the Etheridge family with a device that allows them to live at home as a family without the constant risk or worry of a life-threatening health scare,” says Jenn Hinkle, co-founder and executive director of the Ollie Hinkle Heart Foundation.
Getting the AED in the fall of 2020 has allowed the family to be proactive in managing their shared condition, says Etheridge.
And, most importantly, it’s helped Lynnleigh and Grayson to live like normal kids.