On September 20, 2012, Brandie and Dustin Stoddard welcomed their second baby girl into the world. Haevyn Delanie weighed-in at a healthy seven pounds, two ounces, was 18 inches long, and went home right on schedule.
Just four months later, though, her family was back in the hospital. This time, they were in Kansas City, waiting for a team of medical professionals to transport their critically ill baby to St. Louis Children’s Hospital.
“In her four months, she had never had a fever, never even had a runny nose,” Brandie remembers.
But on January 17, when Brandie picked Haevyn up at daycare, she knew something was terribly wrong. Her baby girl was lethargic, her breathing labored, and, “She was the palest shade of white.”
Rather than wait even a few hours for an appointment, the pediatrician suggested they take Haevyn straight to the emergency room.
“In the chest x-ray, it looked like her heart was taking up half of her chest.”
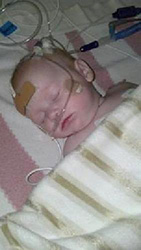 Haevyn’s condition rapidly deteriorated, until her doctors decided Extracorporeal Membrane Oxygenation (ECMO)would be the baby girl’s best option.
Haevyn’s condition rapidly deteriorated, until her doctors decided Extracorporeal Membrane Oxygenation (ECMO)would be the baby girl’s best option.
ECMO is an advanced treatment that uses a pump and oxygenator to deliver oxygen to vital organs – doing the work in place of failing heart and lungs.
After a few days, though, they didn’t see enough of an improvement.
“Since her heart was so sick, they recommended we get to St. Louis because they could offer support that wasn’t available in Kansas City.”
Transporting a child on ECMO, however, is a very delicate task, and offered by only a handful of pediatric hospitals. St. Louis Children’s had only launched the service in late 2012. Haevyn would be the team’s second ECMO transport.
Each specialized trip requires the expertise of an attending physician, two nurses and a perfusionist. While the physicians and nurses balance the patient’s condition and medication needs, the perfusionist operates the heart-lung machine. On this trip, Mark Shepard was responsible for transferring Haevyn from one ECMO circuit to another.
“We received the call about Haevyn on a Monday,” Shepard recalls. “So our team got together and made a plan to get to Kansas City the next morning. We were wheels up in St. Louis at 8:15 a.m.”
They arrived in Kansas City within two hours.
“When we walked into the room, I saw Haevyn’s mom sitting in the corner, worried to death. I went over and talked over everything as we went through it, reassured her that we knew the routine. We’d been in this ICU. Everyone knew their roles.”
Their process worked. Hours after they arrived, Haevyn was on KidsFlight 3, St. Louis Children’s Hospital’s fixed-wing aircraft. Her parents began the drive from Kansas City before the plane carrying their daughter was off the ground.
“I was so sick the entire ride,” Brandie remembers. “I knew she was being sustained by a machine. I knew she was in good hands. But I also knew I couldn’t hold her, and that was hard.”
They were half way to St. Louis when a Cardiac Intensive Care Unit (CICU) nurse called to say Haevyn had done well with the flight, and was getting settled in the unit. That was 16 hours after the transport team first left St. Louis.
“It’s a long day for everybody,” Shepard says. “But it’s so rewarding when you see a patient transferred as successfully as Haevyn was.”
Haevyn arrived in St. Louis on Tuesday, January 22. Doctors told the family that the longer she was on ECMO, the more likely Haevyn would develop complications. They listed her for heart transplant the following Friday. And after a series of ups and downs, her team determined it was time for a solution that could provide more long-term support while she waited for a new heart. On February 14, Haevyn received the ultimate Valentine. That was the day she received her Berlin Heart, a Ventricular Assist Device (VAD) that would function in place of her heart for longer than ECMO.
Exactly four weeks later, Haevyn was offered a new heart. Shepard saw the family that morning.
The surgery went beautifully. The Stoddards were able to leave the hospital ten days later. “Mom was terrified the day she arrived at the hospital. But the day of the transplant, she was so happy.”
Monitoring her from transport to transplant, Shepard became a barometer for Haevyn’s progress.
 “The child we had to take out of Kansas City on a stretcher left here in a stroller with her parents.”
“The child we had to take out of Kansas City on a stretcher left here in a stroller with her parents.”
Two months later, Haevyn is back home in Kansas.
According to her mom, “She’s the same happy baby now that she was before she got sick. She’s catching up on her developmental milestones, and everything looks good!”
“That’s what the program was designed to do,” Shepard says. “That makes you feel like the entire program works. Success like this is what makes us want to get up and get to work.”








