St. Louis Children’s and Washington University Heart Center offers patients and families medical and emotional support
“It felt like the world fell out of my body.”
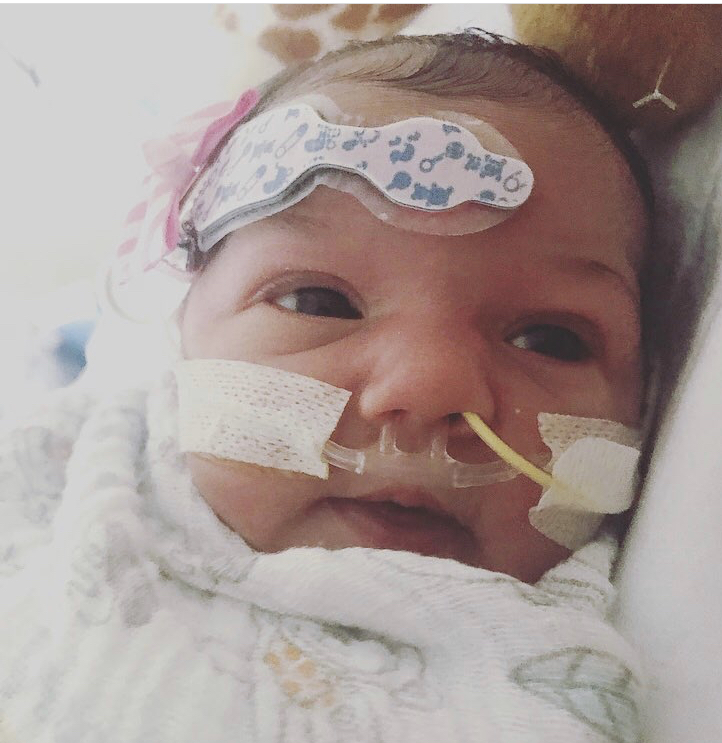 That was the first reaction Salem Prestien had when she learned at 22 weeks into her second pregnancy that her daughter, Lilia, would be born with a single ventricle heart defect.
That was the first reaction Salem Prestien had when she learned at 22 weeks into her second pregnancy that her daughter, Lilia, would be born with a single ventricle heart defect.
As the mom of a young son, Henry, born in 2017 with medical complications, Prestien was overwhelmed by the news about her daughter and knew her family was going to need to make changes.
“We decided that since our son already required lots of specialty care and our daughter was going to, as well, that we would move to St. Louis,” Prestien recalls. She and her children’s father, Nicholas, made the decision to leave their home and family in Springfield, Mo., to be closer to Barnes-Jewish Hospital, where Prestien delivered Lilia on Oct. 2, 2018, and St. Louis Children’s Hospital, where specialists could provide care for both children.
The St. Louis Children’s and Washington University Heart Center is a welcome support for families like Lilia’s when a baby has been diagnosed with a heart defect. The center’s specially trained pediatric cardiologists, surgeons, neonatologists and other experts in pediatric heart specialties provide comprehensive care for these young patients.
Whether diagnosed prenatally or following the baby’s birth, Heart Center patients and their families are provided care through a continuum of services that can include the Fetal Heart Center, High-Risk Cardiac Infant Program, Cardiac Neurodevelopment Program and the Perinatal Behavioral Health Service.
Prenatal heart care and beyond
 Lilia’s care was followed prenatally by the Fetal Heart Center, and Prestien’s high-risk pregnancy was managed by the Fetal Care Center, a partnership among St. Louis Children’s Hospital, Barnes-Jewish Hospital and Washington University Physicians.
Lilia’s care was followed prenatally by the Fetal Heart Center, and Prestien’s high-risk pregnancy was managed by the Fetal Care Center, a partnership among St. Louis Children’s Hospital, Barnes-Jewish Hospital and Washington University Physicians.
“We coordinate appointments with the Fetal Care Center and our high-risk OB/Gyns who work in maternal/fetal medicine. We offer tours of our cardiac intensive care unit (CICU) or newborn intensive care unit (NICU) depending on where we think their baby will go after delivery,” explains Kym Galbraith, RN, BSN, Fetal Heart Center nurse coordinator. “For different diagnoses, we will consult with our pediatric advanced care team — a medical team comprised of a pediatrician and two nurse practitioners — who really focus on the family aspect of having a complex medical child and their desires for their family. It’s important for our families to have an understanding about what life will look like, not only just in the immediate newborn period but what to expect later.”
There are three main cardiologists who do fetal consults and will follow mom and baby throughout pregnancy, says Caroline Lee, MD, director of the Fetal Heart Center and a Washington University pediatric cardiologist.
“Our goals are to confirm diagnosis, look for any changes or evolution of the heart defect over the course of the pregnancy and, more importantly, to counsel step-by-step and prepare families for what to expect emotionally and for their baby’s medical care,” says Dr. Lee, adding that the center provides patients an appointment as soon as possible after their OB has indicated there may be a heart defect.
After arriving in St. Louis, Prestien and Lilia continued to be closely followed by the Fetal Care Center.
“I had no issues with my delivery, and Lilia went straight to the cardiac intensive care unit (CICU), where she stayed for 15 days and underwent two cath procedures. She had a stent placed in her pulmonary valve to get her through until she was big enough for her Glenn procedure (the second of three surgeries typically associated with a single ventricle anatomy),” Prestien says. “She’ll have additional surgeries as she gets bigger, including the Fontan when she is 3 or 4 years old.”
Lilia is moving through the continuum of care provided through the Heart Center and its specialized programs.
“The world of congenital heart defects is so varied — no two hearts are the same, so no one’s experience is the same. The Fetal Heart Center taught me exactly what I needed to know about Lilia’s diagnosis and how to care for her,” Prestien says. “They were amazing and so supportive.”
Monitoring baby through high-risk infant interstage monitoring program and neurodevelopment
 Following Lilia’s birth, her progress was monitored by the Heart Center’s High-Risk Cardiac Infant Interstage Monitoring program, which helped her family prepare for going home.
Following Lilia’s birth, her progress was monitored by the Heart Center’s High-Risk Cardiac Infant Interstage Monitoring program, which helped her family prepare for going home.
As a nurse coordinator for the Heart Center, Julie Stumpf, RN, MSN, worked closely with Lilia’s family to prepare them for discharge and help them through the interstage period between her first surgery and her second surgery, the Glenn procedure, which she underwent in May 2019.
“During this interstage period, our patients are followed closely during a four-month to one-year period,” Stumpf says. “Every two to four weeks, they have clinic visits. There is also home monitoring, which includes parents calling twice weekly to track growth, oxygen saturation, feeding and overall progress. We talk to our families at least twice a week just to make sure they are doing OK.”
Prestien says having this interaction with Stumpf was invaluable.
“We didn’t meet Julie until after Lilia was born and in the CICU, but she’s the one that gave us all the information we needed to care for her at home,” she says. “She was the point person for everything and always responded when I’d text just to make sure things were normal. She was really my fairy godmother and has always been there for us.”
In fact, Stumpf has continued her follow-up with Lilia and her family through the Heart Center’s Cardiac Neurodevelopmental Program, which was established to help infants and children with heart disease reach their highest potential.
“We have worked really hard as a program to have a recognition and awareness of neurodevelopmental care, starting before birth through admission to the CICU and throughout their care,” Dr. Lee says. “Rounds are done by a developmental team of therapists, dietitian, nurses and neurologist who focus on the baby’s development throughout their hospitalization.
“After these children have left the hospital, we ensure they are set up for neurodevelopmental follow-up through the outpatient clinic because it’s increasingly recognized that children with congenital heart defects are at risk for developmental delays,” she adds.
Most patients are first seen in the Cardiac Neurodevelopment Clinic between the ages of 3 to 6 months to establish a baseline.
“In this clinic, we really focus on early assessment and recognition of developmental delays,” Stumpf says. “As a multidisciplinary clinic, our patients can see cardiologists, advanced practice nurses, specialists in neurology, newborn medicine, psychology, neuropsychology and a variety of therapists.”
Lilia was first seen in the clinic at about 6 months and will have another evaluation at 9 months.
“She’s doing really well. Her development is a little behind physically, but she is learning to do all of the normal things like eat table food, roll over and sit up,” Prestien says. “She seems happy to me and seems to understand that she’s better.”
Caring for the whole family
 Caring for Lilia and her son is a full-time job for Prestien and sometimes it is hard to remember to take care of her own well being. This is often true for families who learn that their children will require specialized care, and many families experience feelings of anxiety and worry that can be overwhelming.
Caring for Lilia and her son is a full-time job for Prestien and sometimes it is hard to remember to take care of her own well being. This is often true for families who learn that their children will require specialized care, and many families experience feelings of anxiety and worry that can be overwhelming.
To help provide additional emotional support as they navigate their baby’s care, the Heart Center provides a dedicated therapist to parents through the Perinatal Behavioral Health Service team at Washington University. Families are typically referred to the program by obstetricians, nurse coordinators and social workers.
“While pregnancy can be a wonderful time for families, when a baby is experiencing a medical complication such as a congenital heart defect, there can be additional stress that families were not anticipating,” says Lauren Weir, MA, LPC, staff therapist. “Every time a family is diagnosed during pregnancy, that referral comes to me so I can reach out to families and use an evidence-based tool to screen mom for perinatal mood and anxiety disorders.”
Weir is then available to follow them through the rest of their pregnancy and the postpartum period, when most of these babies are hospitalized.
Weir often meets one-on-one with moms either in the hospital setting, an outpatient clinic and by phone when needed. She also provides support for any family members and other caregivers, if needed.
“I began seeing Lauren regularly before and after Lilia was born and continue to see her,” Prestien says. “It’s important for me because all of my family is out of town. Having someone like Lauren who understands what it is to go through something like this and can help put the pieces together and bounce your thoughts off of has been abundantly helpful.”
Weir encourages families to understand the importance of mental health during this time. 
“I want parents to understand the importance of taking care of themselves — whether it is finding time to be alone even for a half-hour in another room, getting into a sleep routine and making healthier choices when it comes to eating and exercise when possible,” Weir says. “The analogy I often give is when you are on an airplane and they encourage you to put on your own mask first before you can help anyone else. We care very much about our patients, and we want to make sure we are caring for the whole family.”
Stumpf agrees and says she encourages families to ask for help whether for their children or themselves. “I have so much respect for all of our families. They go home with children who are very complex and they have to be equipped and taught how to care for them,” she says. “It’s a huge accomplishment for these patients and their families. It’s why we are here to help them. We are on this journey with them.”