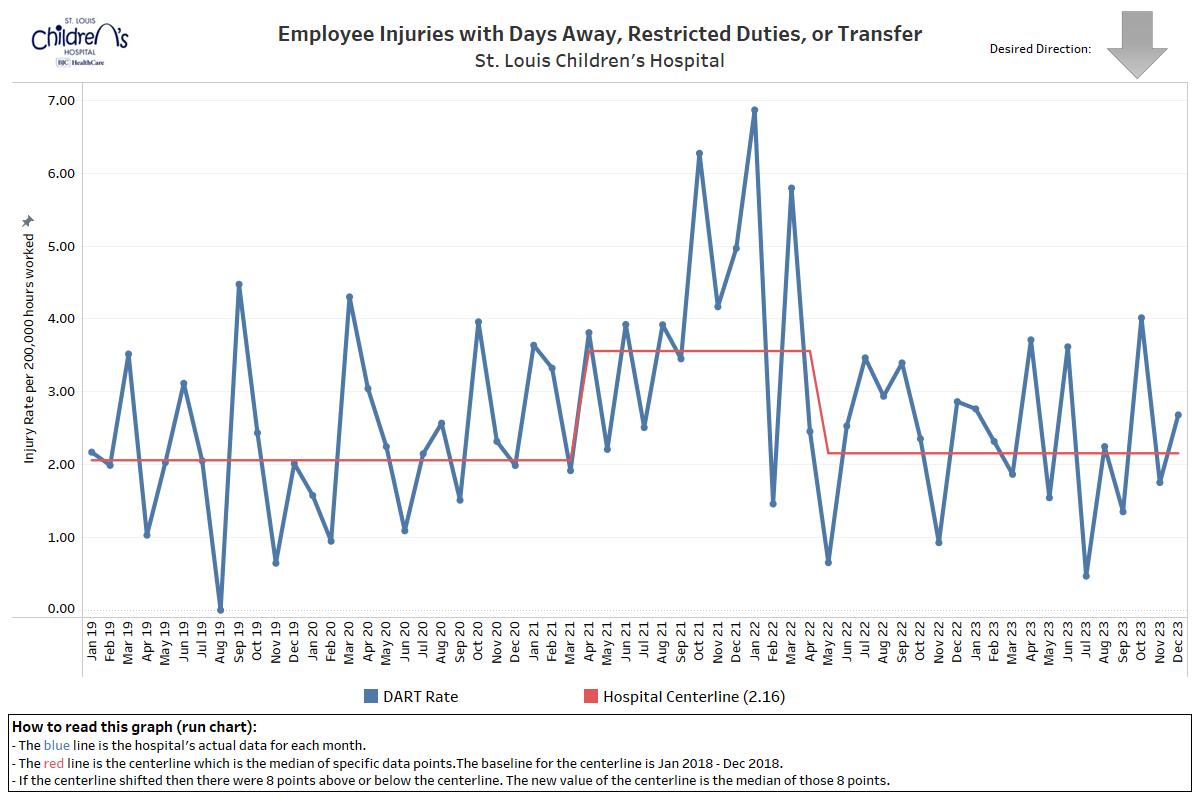
What is a workplace injury with days away, restrictions, or transfer (DART)?
This refers to how many injuries or illnesses on-site lead to workers taking time off, being restricted to certain tasks, or transferred to another role.
If an employee is injured at work and he/she misses days of work, has to restrict his/her work activity, or temporarily transfer to a different job, it is a DART injury.
Why do we measure the number of workplace injuries?
Tracking employee injuries helps us monitor the overall health and safety culture within our organization as well as giving us the ability to analyze data and metrics over time to identify areas of concern and opportunities for improvement.
By monitoring our DART rate, it helps employers determine how many workplace injuries and illnesses caused employees to miss work days, perform restricted work activities or transfer to another job within one calendar year. DART injuries tend to be more of our severe injuries, so it is important to track this data.
This safety metric helps us determine how many workplace injuries and illness required employees to miss work, perform restricted work activities, or transfer to another job within a calendar year.
By tracking where and how these injuries happen, we can take steps to prevent future injuries and keep employees safe at work.
How we measure:
The number of recordable injuries that require employees/staff to take time off from their job, do lighter (restricted) duties or be transferred to another job as defined by OSHA’s DART definition per 200,000 number of hours worked.
What are we doing to improve?
- Developed SLCH Safety Goals and provided them to every employee.
- Published monthly SLCH Regulatory and Safety Newsletter to inform staff about hospital industry regulatory and safety issues.
- Implemented SLCH Safety Cross to discuss the previous day’s employee injuries or incidents during unit and leadership huddles.
- Provided bi-weekly hospital and department education based on injury and incident trends in the hospital.
- Developed action plans to reduce department-specific injuries and incidents.
- Developed safety training presentations for staff based on leading hazards in the workplace.
- Provide monthly and quarterly department injury reports to department directors and managers.
- EHS Department reviews department injury reports with department directors and managers to ensure safety matrices are being met.
What can employees do to help prevent workplace injury or illness?
- Discuss employee safety concerns during departmental meetings.
- Report unsafe conditions or unsafe acts in the hospital by contacting Environmental Health & Safety (EHS):
- Phone: 314.393.4506
- Email: [email protected]
- Educate and train other employees on specific safety hazards in the workplace.
- Provide the proper personal protective equipment (PPE) and ensure that it is being used.
- Ensure good housekeeping standards are being met to prevent unintentional workplace injuries or incidents.
- Use situation awareness when performing job tasks.
This is what has been done and continues to be done over the last several years in addition to what’s listed above.
Employee Injury Prevention Strategies
- Interactive employee Injury metrics are pushed out to managers via Tableau monthly with departmental and hospital wide safety statistics.
- Create department safety teams/committee to implement 2023 employee injury reduction program.
- Departmental employee injury reduction actions plans created and reviewed with staff and managers
- Conducted injury investigation and review with staff/managers.
- Provide employee safety education to staff to reduce injuries.
- Complete task safety analysis and develop job hazard analysis around tasks that contribute to muscle strains, striking stationary objects, and proximity of sharps containers to patient care areas.
- BH Personal Protective Equipment (PPE) researched and supplied to the floors in areas with patients with behavioral health needs to protect staff.
- BH PPE Carts purchased to provide just in time access to PPE given the impulsive nature of BH WPV incidents.
- Conduct Environmental Risk Assessments for patients with BHB
- Provide hospital wide Safety Alerts that identify unsafe conditions to prevent injuries.
- Pediatric Behavioral Health Unit (PBHU) created to treat non-violent patients with Behavioral Health (BH) needs due to open milieu
- Implemented multidisciplinary Behavioral Health rounding to better understand Behavioral Health patients’ tendencies and triggers and effectively communicate to nursing staff a Behavioral Health plan individualized for each patient.
- Reallocated existing positions to improve processes for placing BH patients to decrease length of stay
- Crisis Prevention Institute leadership and subgroups created to create action items across multidisciplinary departments and roles.
- Evaluated and implemented successful mitigation programs from other Hospitals. BH TEAM has learned from Children’s Hospital Association webinar and Patient Safety Organization Safe Tables and reached out to Cincinnati and Boston Children’s to learn their programs/interventions. What we learned is many centers don’t have as many violent pts as we do.
- Employee injury metrics pushed out to managers via Tableau monthly with departmental and hospital wide safety statistics.
- Moved from Safe Tactics and Responsible Restraints (STARR) to Crisis Prevention Institute Program (CPI) response training.
- Created emergency BH PPE kits/bags stored in Occupational Health to be accessed at any time if a BH patient is brought to a department with limited or no BH PPE resources.
- Issued personal duress alarms to all SLCH staff who desired them.
- Create a Standard Work Program to ensure a safe environment while caring for patients with behavioral heath needs.
- Incorporating behavioral health personal protective equipment into CPI training classes to better educate and familiarize staff on proper use. Soliciting real time feedback to modify Personal Protective Equipment types.
- Ongoing training and education through safe, hands-on mock Crisis Prevention Institute training with real scenario events.
- Complete the Emergency Department Safety Expansion (May 2022).
- Implementing a community officer program where officers are stationed in areas where patients with BH needs who are exhibiting violent and/or high-risk behaviors.
- Enable the use of a crisis prevention team that utilizes unit-based verbal de-escalation techniques prior to a CPI being called
- Implementing improved elopement precautions (lock down capabilities at the unit level, and delayed egress with camera coverage at all exit stairwells.
- Continue to modify designated BH inpatient rooms on units to reduce injury risk to patients/staff.